From GP to C-Suite: How Emerging Healthcare Careers are Disrupting Traditional Careers
From GP to C-Suite: The Emerging Healthcare Careers: How Business Models Are Reshaping Health Jobs
Healthcare careers are evolving rapidly as business models shift from traditional clinical roles to strategic leadership and digital innovation. Discover emerging jobs, industry changes, and what hospital executives and HR need to know to recruit and retain top talent.
Introduction
The healthcare industry is undergoing profound transformation and what it means to work in health. Careers that followed a relatively predictable path, from clinical training to lifelong practice in a hospital or private clinic are evolving. Traditional models of medicine, where doctors primarily practiced in hospitals are moving into complex, fragmented ecosystems driven by more business-oriented digital innovation, corporate consolidation, and new care delivery models. Healthcare executives and human resource leaders are now navigating a complex workforce environment. It is not just for recruiting, but for building a workforce that can adapt to the future of care. Understanding these shifts is critical, not only to stay competitive in recruiting top talent but also to lead their organisations through change.
This post explores how these changes are unfolding, with examples of new job pathways, industry-wide trends, and implication for recruitment and retention in hospitals and health organisations as healthcare business models reshape health careers.

The Shift in Healthcare Business Models
From Clinic to Complex Ecosystem
Historically, healthcare careers revolved around direct clinical care in hospitals and private clinics delivered primarily through:
Public hospital systems, funded and structured through government frameworks.
Private specialist and general practice clinics, often owned and operated by doctors.
Fee-for-service models, where remuneration depended on the number of patients or procedures.
However, over the past two decades, several forces have disrupted this model where deliver is integrated across sectors (hospital, primary care, virtual platforms), supported by technology (telehealth, AI diagnostics, remote monitoring), and funded through complex mixes of public/private investment, including private equity buyouts.

This model has increasing given way to a more corporatised, digitally enable structure, where deliver is through:
- Commercialisation and Consolidation: Private equity and corporate groups now own many clinics and specialty practices. For example, large healthcare companies like Healius and Sonic Healthcare have acquired thousands of clinics across Australia, turning doctor-owned practices into employee-run entities (Australian Financial Review, 2023).
- Digital Health Revolution: Telehealth, AI diagnostics, remote monitoring, and virtual care platforms are transforming service delivery. The COVID-19 pandemic accelerated adoption of these technologies, creating roles beyond clinical practice (Australian Government Department of Health, 2022).
- Policy and Funding Shifts: Governments and insurers increasingly support value-based care models, prioritizing outcomes over volume, reshaping the way care is funded and delivered (Commonwealth Fund, 2024).
These changes shift the operational, financial, and workforce dynamics of healthcare organisations. And they open new pathways for professionals who blend clinical expertise with leadership, strategy, or innovation experience.
Fragmentation of Medicine: Multiple Employers, Multiple models
This business model shift has fragmented medicine into multiple entities — hospitals, insurer-backed care programs, tech startups, government health bodies, and corporate health services, each requiring different skills and roles. Clinicians increasingly move into roles that blend medicine, business, technology, and governance
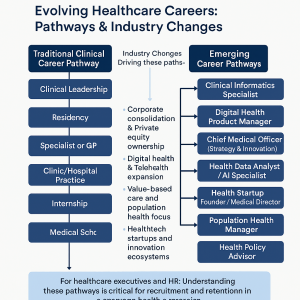
New and Emerging Healthcare Jobs
As the ecosystem fragments and digital innovation grows, new career paths emerge alongside traditional clinical roles. Medicine is no longer confined to the hospital ward or clinic. Today, doctors, nurses and allied health professionals might work for:
Health startups and digital platforms.
Government policy teams or public health departments.
Insurers and funders designing care models.
Corporate-owned clinics or virtual hospital networks.
Each of these sectors has its own culture, objectives, and job expectations. For HR teams, this means rethinking how jobs are defined and how healthcare professionals are recruited and retained.

Examples of Emerging Roles
- Chief Medical Officer (CMO) as Strategic Leader
Once focused on regulatory compliance and clinical governance, CMOs are now expected to contribution to central to strategic decision-making, digital transformation, innovative leadership, and organisational growth. They play bridge clinical expertise with business acumen and digital transformation leadership (Healthcare Executive, 2023).
They play key roles in guiding hospital or health system direction, often with a focus on outcomes, experience, and cost-efficiency. Healthcare Executive: The Evolving CMO - Clinical Informatics and Digital Transformation Leads
As hospitals digitise their workflows and adopt tools like electronic medical records, AI decision support, and predictive analytics, clinicians with data and informatics knowledge are in high demand. This role is growing quickly within hospital networks and national digital health initiatives. These professionals integrate clinical knowledge with data analytics and IT to improve patient outcomes through technology, supporting hospitals’ digital strategies (AMIA, 2024). - Medical Directors in Health Startups
Health startups and digital platforms require clinicians who understand both medicine and product development to guide innovations that are clinically effective and user-friendly. Doctors and senior nurses often work as medical directors, advisors, or consultants in companies building AI tools, remote monitoring apps, or virtual care platforms (Rock Health, 2024). - Health Data Analysts and AI Ethics Specialists
With massive volumes of health data now available, organisations need professionals who understand both clinical care and data science. Doctors are stepping into hybrid roles focused on interpreting data for service improvement and managing the ethical implications of machine learning in diagnosis. These roles use clinical and health data to develop predictive models, improve diagnostics, and inform policy decisions, often working closely with clinical teams (Nature Digital Medicine, 2023). - Care Coordinators and Population Health Managers
As care becomes more community-based and outcome-driven, new roles are emerging to manage chronic disease across populations, coordinate care transitions, and ensure equity in service access. These positions often sit within integrated health networks or community health organisations. These professionals manage patient journeys across providers and technologies to optimise outcomes and costs (CDC, 2024).

Industry-Wide Changes Shaping Healthcare Careers
- Corporate Consolidation of Clinics and Hospitals
Private equity’s entrance into healthcare has shifted many doctors from owners to employees or contractors. Corporate players are increasingly buying up general practices and specialist clinics. This centralisation of ownership changes work conditions for clinicians and creates new leadership, operational, and compliance jobs. This leads to new management roles, compliance officers, and clinical governance positions that require medical expertise alongside leadership skills (Harvard Business Review, 2023).
- Expansion of Digital Health
Digital-first care models, including virtual hospitals, 24/7 telehealth platforms, and AI-enabled triage systems, are normalising remote work and creating jobs that didn’t exist a decade ago. This expands the career options for both clinicians and non-clinical professionals with healthcare knowledge. Dgital transformation creates demand for cross-disciplinary professionals combining medicine, IT, data science, and business. Hospitals now employ clinical informaticians, telehealth coordinators, and AI ethics officers (McKinsey & Company, 2023).
- Growth of Integrated Health Networks and Value-Based Care and Preventive Focus
Governments and insurers are shifting funding models to reward prevention, coordination, and patient outcomes. This requires skills in data interpretation, cross-sector collaboration, and long-term care planning. As a result of health systems grow they will increasingly require roles in population health, care pathway design, health economics, quality improvement, and care coordination to manage outcomes under new funding models. This creates positions in clinical leadership with a focus on strategy and operations (Health Affairs, 2024).

Recruitment Implications for Executives and HR?
Recruitment Challenges and Opportunities
The widening scope of health jobs means that recruitment strategies must also evolve. Key considerations for HR and executive leaders include:
Broader job definitions: Candidates may come from health startups, academia, or policy — not just hospitals.
Expanded skill requirements: Beyond clinical experience, employers now seek digital capability, adaptability, leadership, and a strategic mindset.
Retention planning: High-performing professionals increasingly want mission-driven work and influence in strategy, not just service delivery.
Health organisations that understand and reflect these expectations will be more competitive in attracting top leadership and clinical talent with:
- Broader skillsets required: Hiring now involves evaluating clinical expertise plus leadership, digital literacy, and strategic thinking.
- Diverse candidate pools: Candidates come from non-traditional backgrounds, including tech startups, public health, and policy sectors.
- Retention: Doctors in leadership roles expect meaningful involvement in strategy and innovation, not just compliance.
How Health Jobs Platforms Can Help
Specialised career platforms play an essential role in this shift, acting not only as recruitment tools but as hubs of information and insight for executives, HR, and clinicians navigating this changing healthcare environment.
- Serve as a central hub for leadership insights and career developments.
- Facilitate targeted recruitment for emerging roles beyond clinical care.

Conclusion: What the Shift in Healthcare Careers Means
Healthcare careers are no longer linear or confined to clinical spaces. The business model of healthcare has shifted from doctor-owned clinics and centralised hospitals to networked, tech-enabled, commercially complex systems.
This change is driving a diversification of health job roles, where strategy, technology, and innovation are just as critical as clinical care. Healthcare professionals, particularly those with leadership potential, are seeking careers that let them shape health systems, not just deliver services within them.
For hospitals and healthcare organisations, this is a turning point. Workforce planning, job design, and recruitment must now align with a redefined health environment, one that values cross-functional expertise, flexibility, and system-level impact.
Healthcare executives and HR leaders must stay ahead of these evolving career environments to attract and retain top talent
References
- Australian Financial Review, 2023: Healius and Sonic Healthcare acquisitions
- Australian Government Department of Health: Telehealth initiatives
- Commonwealth Fund, 2024: Value-based care models
- Healthcare Executive, 2023: CMO evolution
- AMIA, 2024: Clinical informatics
- Rock Health, 2024: Digital health state report
- Nature Digital Medicine, 2023: AI in health
- CDC, 2024: Population health management
- Harvard Business Review, 2023: Private equity in health
- McKinsey & Company, 2024: Digital health transformation
- Health Affairs, 2024: Integrated care models

. Visit UBIS Health Jobs + Careers
Provide careers+jobs and ongoing education about industry trends to executives and HR. Explore leadership opportunities, post strategic roles, and access expert insights on healthcare workforce trends shaping tomorrow’s health systems

